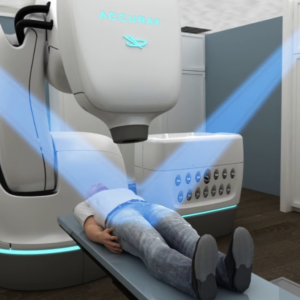
Combining stereotactic body radiation therapy (SBRT), such as CyberKnife with standard systemic therapy yielded significant increases in the rates of biochemical response and progression-free survival (PFS) in patients with oligometastatic castrate-resistant prostate cancer (CRPC), the phase II randomized ARTO trial showed.
In a cohort of 157 patients at 6 months after the start of treatment, biochemical response was detected in 92% of those who received SBRT with abiraterone acetate (Zytiga) and prednisone versus 68.3% of those treated with standard systemic therapy alone (OR 5.34, 95% CI 2.05-13.88, P=0.001), reported Giulio Francolini, MD, of Azienda Ospedaliero Universitaria Careggi in Florence, Italy, and colleagues.
Complete biochemical response was observed in 56% of patients in the experimental arm versus 23.2% of those in the control arm (OR 4.22, 95% CI 2.12-8.38, P<0.001), they noted in the Journal of Clinical Oncology
After a median follow-up of 24.9 months, median PFS was not reached in the experimental arm versus 17 months in the control arm, translating to a significantly reduced risk of progression with SBRT (HR 0.35, 95% CI 0.21-0.57, P<0.001).
“Median follow-up was long enough to suggest that these results are reliable and deserve attention, especially considering their magnitude,” Francolini and colleagues concluded. “Phase III trials are warranted to test survival endpoints in larger cohorts.”
The addition of SBRT also led to significant benefits in biochemical PFS (HR 0.33, 95% CI 0.16-0.67, P=0.002) and radiologic PFS (HR 0.39, 95% CI 0.19-0.81, P=0.011).
Overall, 24 patients died (nine in the experimental arm and 15 in the control arm). Median overall survival (OS) was not reached in either treatment arm, but there was a nonsignificant OS trend in favor of the experimental arm (HR 0.65, 95% CI 0.28-1.49).
Regarding safety, grade 1 and 2 adverse events (AEs) occurred in 64% and 65.8% of patients in the experimental and control arms, respectively. Grade >2 AEs occurred in 10.6% and 15.8%.
Most toxicities, including blood test abnormalities, fatigue, hot flashes, and hyperglycemia, were mild and related to systemic treatment, the authors noted.
Osteoporosis/fractures, hematuria, and gastrointestinal disorders were AEs considered potentially related to SBRT, with osteoporosis or fracture reported in two patients in the experimental arm and five in the control arm, hematuria in four patients in each arm, and gastrointestinal disorders in two patients in the experimental arm and one in the control arm.
Cardiovascular disorders were reported in 13.3% and 17% of patients in the experimental and control arms, respectively.
Jessica Wong, MD, MEng, of the Fox Chase Cancer Center in Philadelphia, told MedPage Today that while new systemic therapies such as abiraterone and prednisone, as well as radiation techniques such as SBRT, have been able to improve outcomes for men with oligometastatic prostate cancer, “these treatments have not been compared directly in trials and the ARTO trial is the first to evaluate the synergistic effect of SBRT and AAP [abiraterone and prednisone] in men with oligometastatic prostate cancer.”
“This trial showed that adding SBRT to systemic therapy including AAP improved progression-free survival as compared to AAP alone, without increasing the rate of adverse events,” noted Wong, who was not involved in the study. “This shows that SBRT is safe and effective for treating oligometastatic prostate cancer concurrently with new systemic therapy agents.”
The study was conducted at 16 Italian centers and enrolled 157 patients (median age 74 years) from January 2019 through September 2022. Patients had to have metastatic CRPC with three or fewer bone or nodal metastatic lesions.
They were randomly assigned 1:1 to receive standard systemic treatment with abiraterone/prednisone, or standard treatment plus SBRT to all sites of metastatic disease. Patients were followed every 3 months with prostate-specific antigen (PSA) and complete hematologic blood tests.
The biochemical response rate (defined as the percentage of patients with a PSA decrease ≥50% compared with baseline at 6 months after start of systemic treatment) was the primary endpoint of the trial, while secondary endpoints included complete biochemical response rate (defined as the percentage of patients with a PSA ≤0.2 ng/mL at 6 months after start of systemic treatment) and PFS.
Author: Mike Bassett is a staff writer focusing on oncology and hematology.
CyberKnife is the most advanced form of SBRT available for Prostate Cancer Treatment.
Using image-guided robotics, the CyberKnife can precisely and non-invasively dissolve tumors and other lesions with multiple beams of high-energy radiation, while sparing the normal healthy tissue surrounding the tumor or lesion. This revolutionary prostate cancer treatment has helped save many lives while maintaining patients’ quality of life.
The Benefits of CyberKnife for Prostate Cancer Treatment
The benefits of radiosurgery with the CyberKnife far outweigh any potential risks, which are minimal.
98% Prostate Cancer Treatment Success Rate
Recent studies comparing the CyberKnife Radiosurgery to other modalities such as IMRT, LDR, HDR, Proton therapy and traditional surgery have shown that CyberKnife Radiosurgery is as effective in the treatment of prostate cancer, with only five treatments, and has fewer side effects than other modalities.
Targeted Radiation without Damaging Surrounding Tissue
CyberKnife stereotactic body radiation therapy (SBRT) typically emits 150 to 200 small x-ray beams, all penetrating the prostate from multiple angles, resulting in a higher localized dose. The dose targets the exact shape of the prostate, which means a minimal dose of radiation affects surrounding healthy tissue, resulting in much fewer, if any, side effects.
Faster Prostate Cancer Treatment Times
CyberKnife therapy requires only five treatments. Each treatment fraction is a much higher dose than given with proton therapy. This is called hypofractionated treatments.
Proton beams deliver a lower dose of radiation to the prostate, so many more treatments are required to a larger treatment area. These treatments use conventional fractionation with small doses given daily over a four to six week period.
Evidence-Based Prostate Cancer Treatment
A growing body of evidence from clinical studies using CyberKnife hypofractionated radiation treatments (high dose in five treatments) shows that CyberKnife provides more effective treatment compared to the proton beam’s conventional lower dose fractionation treatment.
The most recent ten-year study by Dr. Alan Katz published in the journal Radiation Oncology confirms that using high-dose hypofractionation radiation therapy with CyberKnife is as good as or better than the protected low-dose conventional fractionation treatments with proton beam, and the toxicities to the bladder and rectum are lower using CyberKnife therapy.
Pinpoint Accuracy and Comfort
CyberKnife beams are continually image-guided throughout the entire treatment so the robot adjusts for any slight movement the patient makes. This enables the CyberKnife beam to follow the prostate’s movement even as the patient breathes normally. If the movement is large the CyberKnife will suspend the beam until the patient is back in alignment. This allows for precise targeting of the prostate in an approximately two to five-millimeter area surrounding the prostate.
Proton beam treatments do not have continual image-guided technology, therefore the equipment cannot make adjustments when the patient or the prostate moves, which happens naturally just by breathing. Therefore, a larger treatment area, other than just the prostate, is treated to compensate for this uncertainty. The target is usually the prostate plus 10 to 15 millimeters all around the prostate, which can result in more side effects.
Also, gas bubbles in the intestines and the bladder filling can move the prostate during treatment, sometimes up to 20 millimeters. That’s also why proton treatments rely on a bigger treatment margin to keep targeting the prostate. Since CyberKnife uses continuous image guidance to correct for any prostate motion or patient movement, it can target just the specific pinpointed area.
Listen as Board Certified Radiation Oncologist, Dr. Mark Pomper explains why CyberKnife is a better choice than other types of radiation therapy for prostate cancer.
See our patient stories to read about successful treatments at the CyberKnife Center of Miami. Our staff would be more than happy to discuss the benefits of stereotactic radiosurgery with you. Call CyberKnife Miami today at (800) 204-0455 or you can contact us online.
